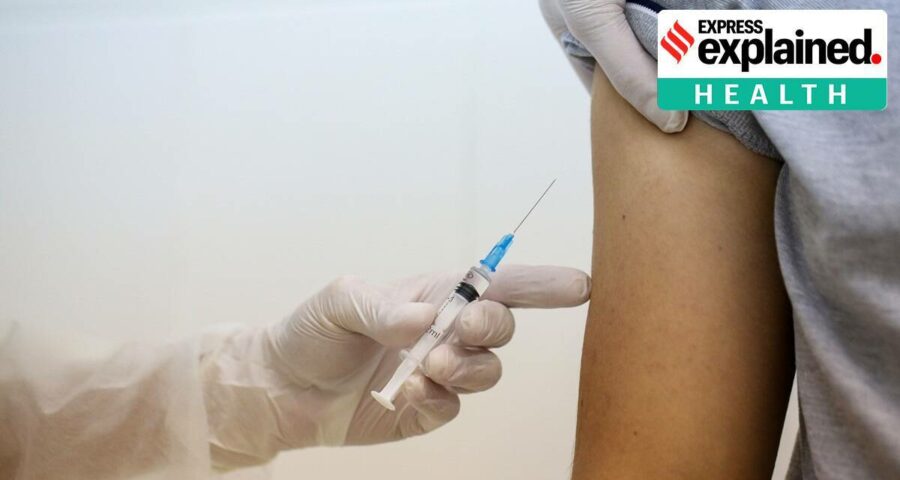
The WHO endorsement paves the way of the use of this vaccine outside the pilot programme, in all areas where malaria is known to be widely prevalent.
The World Health Organisation, on Wednesday, allowed the “widespread use” of the world’s first vaccine against malaria, a common mosquito-borne disease that claims more than four lakh lives every year. Developed by GlaxoSmithKline, the vaccine, known as RTS,S/AS01, has already been administered to nearly 8 lakh children in Ghana, Kenya and Malawi as part of a pilot programme since 2019.
The WHO endorsement paves the way of the use of this vaccine outside the pilot programme, in all areas where malaria is known to be widely prevalent. But the RTS.S/AS01 vaccine, known by its brand name of Mosquirix, is considered only the first step towards effective immunisation of global population against malaria. This vaccine is able to prevent severe cases of malaria in only 30 per cent of the cases, and the quest for more effective vaccines is still underway.
Biggest killer
Malaria is known to be one of the deadliest diseases in human history, having claimed millions of lives. Even now, the disease kills over four lakh every year, according to WHO figures. This is still a huge improvement from twenty years ago, when close to double the number of people were succumbing to the disease.
Malaria is most endemic in Africa, with Nigeria, Congo, Tanzania, Mozambique, Niger and Burkina Faso together accounting for over half the yearly deaths.
India is one of the countries badly affected by the disease. Deaths due to malaria has come down sharply in the last few years — officially these are only in hundreds now — but infections continue to be in millions.
Lack of vaccine
Despite decades of research, scientists have been unable to develop an effective vaccine for malaria, though over 20 candidates have entered clinical trials in the last few years.
To date, the best prevention of malaria remains the use of mosquito nets. However, this does nothing to eradicate the disease.
Scientists cite a variety of reasons for the failure to develop a malaria vaccine, the foremost being the complexity of the life-cycle of the malaria-causing parasite, a part of which is spent in the human host.
“The difficulty in developing effective malaria vaccines stems largely from the complexity of the malaria-causing parasites’ life cycle, which includes mosquitoes, human liver, and human blood stages, and subsequent antigenic variations of the parasite. These parasites are also able to hide inside human cells to avoid being recognised by the immune system, creating further challenges,” wrote a group of Australian and Chinese researchers in an open-access journal last year.
“Another challenge faced in malaria vaccine development is that the common human malaria-causing parasite, P. falciparum, is not a rodent pathogen. The most common mouse models of malaria employ the rodent-specific parasite species P. berghei, P. yoelii, and P. chabaudi. These species generate unique pathologies and immune responses. While they are still employed to model various manifestations of human disease, the immune response patterns observed in these models are not fully transferable to humans,” the researchers wrote.
Mosquirix itself is the result of more than 30 years of research and development, and yet has only modest efficacy.
Other scientists, like Navneet Arora, Lokhesh Anbalagan and Ashok Pannu, researchers from Postgraduate Institute of Medical Education and Research (PGIMER) in Chandigarh point to other reasons like the lack of funding and interest in developing a malaria vaccine.
“Because malaria disproportionately affects LMIC (low and middle income countries) lacking the robust health infrastructure, the vaccine manufacturers have little incentive for malaria vaccines and continued targeting vaccines for industrialized world markets,” the three researchers wrote in a paper in an open-access journal last year.
Other scientists have also mentioned that research for malaria vaccine never received the same kind of attention as, say, HIV/AIDS.
Malaria on decline
However, a significant progress has been made in the last few years in reducing the impact of malaria. A few countries have also been able to eliminate malaria, mainly through spray of insecticides to kill the mosquitoes, and cleaning up areas where mosquitoes breed. In the last twenty years, 11 countries have been declared by WHO to have become malaria free, after zero cases were recorded in these countries for three consecutive years. These countries include United Arab Emirates, Morocco, Sri Lanka and Argentina.
In 2019, as many as 27 countries reported less than 100 cases of malaria. Two decades ago, only six countries had less than this number.
Newer vaccines
Several other vaccines are being tested. One of them has also shown some promise. In May this year, a malaria vaccine candidate undergoing phase two trials reported an efficacy of 77 per cent. This vaccine, R21/Matrix M, is a modified version of Mosquirix, and has been developed by researchers at the University of Oxford. Lead researcher Adrian Hill, director of Jenner Institute and professor of vaccinology at Oxford University, had said he believed this vaccine was the first to reach WHO’s goal of at least 75 per cent efficacy.
Dr V S Chauhan, a former director of Delhi-based International Centre for Genetic Engineering and Biology, and well known for his efforts to develop a recombinant malaria vaccine, said R21/Matrix M held a lot of promise.
“This vaccine is definitely a big hope, but it still has to undergo phase three trials,” he said.
Source: Read Full Article